Reimagining the Indian government’s telemedicine platform
 by Dr. Puneet Khanduja, Venkat Goli and Suhird Singh
by Dr. Puneet Khanduja, Venkat Goli and Suhird Singh Feb 10, 2021
Feb 10, 2021 9 min
9 min
This note highlights three key challenges—abuse, availability, and access that telemedicine platforms in India, such as the government’s eSanjeevani, need to address. It also benchmarks eSanjeevani with other global telemedicine platforms and suggests strategies to tackle the prevalent challenges.
1. Background
Toward the end of December, 2020, The Times of India reported incidents of sexual harassment on Indian telemedicine platforms that offer consultations with doctors. The report noted that these platforms “have become sites for sexual harassment of women doctors, with ‘patients’ flashing, masturbating or making lewd conversation in the guise of seeking consultation.” The report went on to state that instead of informing the police of such incidents, the platforms kept it under wraps and implemented additional measures to prevent such incidents, without much success. While the report mentions the misuse of some private platforms, it does not mention whether eSanjeevani, the telemedicine platform of the Government of India where more than 1 million consultations have been recorded until the end of December, faced similar issues.
eSanjeevani had its genesis on 25th March, 2020 when the Medical Council of India (MCI) and NITI Aayog jointly released the telemedicine practice guidelines. These guidelines enable Registered Medical Practitioners (RMPs) to provide healthcare remotely using digital platforms. Soon after, on 13th April, 2020, the Ministry of Health and Family Welfare (MoHFW) launched eSanjeevani, a platform that offers remote health services. Private sector players, such as Practo, 1mg, among others, also rapidly launched their telemedicine services.
Telemedicine is not new to India. As early as 2009, Health Point Services (HPS) launched a telemedicine offering, eHealthpoint (eHP), in Punjab. However, eHP did not gain much traction. A decade later, the delivery of health services online is now an attractive proposition. This was possible through India’s robust telecommunication infrastructure and ubiquitous availability of the 4G network. The low cost of data, a result of competition among telecom players, as well as high mobile penetration also played a major role in this transition. The COVID-19 pandemic further accelerated the need for remote healthcare and consultation.
2. The government’s telemedicine platform: e-Sanjeevani
eSanjeevani seeks to improve access to health services that had been severely curtailed during the pandemic. This was due to movement restrictions imposed during the lockdown and due to the lack of available health infrastructure as a result of COVID-19. The Centre for Development of Advanced Computing (CDAC) developed and launched eSanjeevani in record time. The platform is available in the following two variations:
- Doctor-to-doctor teleconsultations, provided through eSanjeevani Ayushman Bharat–Health and Wellness Centres (AB-HWC): This is deployed in 6,000 HWCs and is served by specialists and doctors in around 240 hubs. More than 20,000 paramedics, doctors, and specialists received training to use eSanjeevani AB-HWC.
- Doctor-to-patient teleconsultations, provided free of cost through the eSanjeevaniOPD platform: eSanjeevaniOPD enables contactless consultations between a doctor and a patient. Approximately 8,000 doctors received training and were onboarded on eSanjeevaniOPD.
As per the Press Information Bureau on 14th December, 2020, the 1 million consultations recorded until December included more than 200,000 doctor-to-doctor consultations and more than 750,000 doctor-to-patient consultations.
3. Addressing the three “As” in eSanjeevaniOPD: Abuse, availability, and access
While it is commendable that the government reacted with alacrity and agility to ensure health services were available in remote areas, the eSanjeevani platform faces three main issues, which are discussed below.
Abuse: The verification process involved in the registration is similar to that of private platforms, which makes eSanjeevaniOPD susceptible to abuse. A patient must register on the platform before they can use it. The two-step process requires a patient to first verify their mobile number through a one-time password (OTP). Subsequently, they must complete a registration form that includes personally identifiable information (PII), such as name, age, biological sex, and address. To simplify the registration process, no proof of identity is requested at the time of registration. This makes it easy for potential abusers to misrepresent their details and enter the platform without being traced back. The OTP verification only serves to confirm whether the patient can access the mobile number provided during registration. It does not provide additional verification features that can enable law enforcement agencies to trace back the number in case of misuse.
One way to address the issue of abuse mentioned in the article of The Times of India is to use Aadhaar verification during the registration process where an OTP would be sent to the mobile number registered against the person’s Aadhaar. However, this would complicate the registration process and as many do not have their Aadhar linked with their mobile numbers, they would not be able to use the platform. Another way to address abuse in the platform would be to match doctors and patients algorithmically, based on biological sex. This will discourage those who sign up to misuse the platform. Users of the eSanjeevani platform confirmed that male patients were matched with female doctors. This could potentially lead to misuse, similar to incidents reported on private platforms. Moreover, as mentioned explicitly in the telemedicine guidelines, consultations should not be anonymous and both the patient and the doctor need to know each other’s identity. This enables the platform to identify any misrepresentations and take necessary action.
Availability: Doctors, particularly women, who have faced such abuse on these platforms may decline to provide online consultations going forward. This would further reduce the availability of healthcare professionals necessary for the platform to function effectively. eSanjeevani already struggles with a shortage of doctors, which is evident by the time it takes for a patient to receive relevant advice after they request a consultation. Patients recounted incidents where doctors were not readily available, which resulted in long waiting times. They mentioned that it sometimes took more than an hour to consult a doctor, with no indication of the time it would take for a doctor to become available.
Although the portal provides patients with an option to select specialist consultation services through a drop-down menu during registration, patients often receive a message stating that the selected service is closed. Patients then try to avail of a general service where the doctor may not be qualified to diagnose the problem, which can lead to an unsuccessful consultation. This suboptimal experience could discourage them from trying to use the platform again. Besides onboarding more doctors, the platform can provide an option for patients to record their symptoms or ailments when they first seek a consultation. The patient can either type it in their chosen language or record an audio message. Using natural language processing (NLP), the platform can then initiate an algorithmic match between a doctor and a patient to reduce unsuccessful consultations.
Access: While telemedicine practice guidelines allow for video, audio, text-based, and asynchronous modes of communication for teleconsultation, the eSanjeevani platform is solely video-based. This requires the patient to have a smartphone or a laptop with an internet connection. The eSanjeevaniOPD application makes remote health consultation accessible to those with such technology. However, it does not solve the problem for digitally excluded individuals and communities, which include those with feature phones that have no internet connectivity or those who do not own a mobile phone. As of October, 2019, approximately half of India’s population was digitally excluded. Even among those who own a mobile phone, 40% remain digitally excluded. Moreover, the patient must also complete the registration forms before they can initiate a teleconsultation and navigate through the appointment process. This requires a knowledge of the English language since the forms and instructions are only available in English. To ensure that such services are accessible to all, governments should set up functional teleconsultation helplines, auto-diallers, text messages, and other asynchronous channels as these modes are permissible under the telemedicine guidelines.
The government can also use community-based digital centers equipped with mobiles or tablets to increase access, such as panchayat (village level government) offices and Self-Help Groups (SHGs). Governments that do not make adequate investments in these channels risk excluding their “digitally limited” segments of the population, thereby depriving them of access to healthcare. This could lead to a situation where the most vulnerable populations with limited access to healthcare cannot access remote healthcare services as well.
4. The way forward: Benchmarking eSanjeevani to global platforms
Besides strengthening eSanjeevani along the lines of the three As discussed above, it can also benefit from offering a wider variety of services similar to other online health platforms based in India and overseas. To reimagine more diversified service offerings on the eSanjeevaniOPD platform, we benchmarked services offered in the teleconsultation space by eSanjeevani, Practo and 1mg in India, Ping An Good Doctor (PAGD) in China, and Amwell and Teladoc in the USA. Some of the services available on these platforms include online consultations, e-health profiles, express drug delivery, health management plans, appointment services, health check-ups, hospital referrals, second opinions, inpatient arrangements, and domestic or overseas medical services (see Appendix-2 for description of the services). The table below highlights the services these platforms provide.
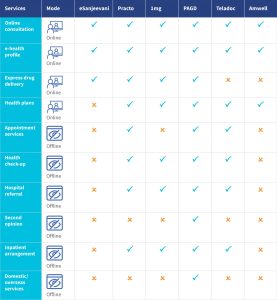
As evident from the benchmarking analysis provided above, there is an untapped opportunity to build eSanjeevani into a world-class teleconsultation platform. This is possible by integrating it within the larger healthcare ecosystem that connects hospitals, clinics, pharmacies, laboratories, diagnostic centers, and doctors who offer in-person consultations. This could be pursued through the National Digital health Mission (NDHM) of the Government of India. However, the government must first address the three “As” of abuse, availability, and access.
Appendix 1: Various health platforms used for comparative study
Practo is a platform based in India that seeks to simplify healthcare by connecting the entire healthcare ecosystem, which includes patients, doctors, pharmacies, diagnostics, clinics, hospitals, and testing labs, among others. Patients can consult doctors virtually and book appointments with them for in-person consultations, order medicines, as well as book tests and check-ups. Practo offers a management software to clinics and hospitals to facilitate activities, such as appointment booking. It enables doctors to create their profiles to increase their online presence and offer online consultations and also allows patients to make appointments for offline consultations. 1mg is another Indian online healthcare service that serves primarily as an online pharmacy. It also offers online consultations and allows patients to book lab tests.
1mg is an online health platform operating in India. 1mg aims to make access to healthcare a hassle-free experience by addressing all health needs of an individual remotely. One can avail of allopathic, ayurvedic, homeopathic medicines, vitamins & nutrition supplements and other health-related products delivered at home. The company also collects samples for lab tests at the patient’s home and provides a platform to consult doctors.
Ping An Good Doctor (PAGD) is a healthcare software company that operates in China, headquartered in Shanghai. PAGD utilizes the internet and artificial intelligence (AI) to address gaps in the Chinese healthcare system. Its objective is to become a one-stop healthcare platform by integrating healthcare information, medical services, drugs, health supplements and equipment, as well as health plans. This includes doctors, hospitals, pharmacies, physiotherapy centers, health check-ups, fitness, beauty care, insurance, and e-commerce. PAGD offers online consultations, e-health profiles, express drug delivery, health management plans, health headlines, centralized appointment services for offline consultation, health check-ups, hospital referrals, second opinion, inpatient arrangements, and domestic or overseas medical services (medical tourism).
Amwell is a telemedicine company based in Boston, Massachusetts that connects patients with doctors over video calls. For healthcare providers, Amwell sells its platform as a subscription service to place their medical professionals online. Its software development kits, APIs, and system integrations enable clients to embed their system into existing workflows.
Teladoc Health, Inc. is a telemedicine and virtual healthcare company based in the US. It provides telehealth services, medical opinions, AI and analytics, and licensable platform services. Teladoc Health uses telephone, video conferencing, and mobile apps to provide on-demand remote medical care.
Appendix 2: Description of the services that have been used for benchmarking telemedicine platforms
Online consultation: Patients can talk to physicians online and consult them through video or voice calls for diagnosis, prescriptions, and other services
E-health profile: Digital version of a patient’s health chart that includes real-time health records, which capture their medical history, diagnoses, medications, treatment plans, immunization records, test results, etc.
Express drug delivery: Medicines can be delivered to patients soon after a consultation, through a delivery platform
Health plans: Customized health plans based on e-health profiles of patients
Appointment services: Booking of appointments through a centralized system
Health check-up: Thorough physical examination, including a variety of tests based on the age and health of a person
Hospital referral: After consultation with a physician, if more advanced care is required, the doctor can refer the patient to a hospital
Second opinion: After an unsatisfactory diagnosis, a patient can request to consult a different doctor for a second opinion
Inpatient arrangement: Arrangement for admitting patients to a hospital for surgery or other procedures
Domestic/ overseas services: Travel arrangement for patients who wish to travel to a different location for medical treatment or care



Leave comments