NFHS 5 calls for urgent action on child nutrition in India
 by Aakash Mehrotra, Dr. Puneet Khanduja, Monica Dutta and Palak Khanna
by Aakash Mehrotra, Dr. Puneet Khanduja, Monica Dutta and Palak Khanna Feb 11, 2021
Feb 11, 2021 7 min
7 min
The article highlights findings from the first round of National Family Health Survey (NFHS) 5, a large scale nationwide survey of households in India, released in Dec’20. The article primarily focuses on Five major indicators of child nutrition and compares the outcome of first round of NFHS 5, covering 54% of India’s population with previously conducted NFHS, 3 and 4 in the year 2005-06 and 2015-16 respectively.
The percentage of children who are stunted, wasted, underweight, anemic, and obese is on the rise across India. Despite impressive progress in areas, such as water and sanitation—immunization and maternal health indicators of child health alongside nutrition remain a matter of grave concern. UNICEF predicts a further increase in malnutrition by at least 10% in the country, as a result of the COVID-19 crisis.
The Ministry of Health and Family Welfare, Government of India has recently released a report on findings from the first round of the Fifth National Family Health Survey (NFHS 5). The survey covers 17 states and five union territories, which comprise 54% of India’s population, and informs policy on household-level health and nutrition indicators. Since the NFHS is an outcome-level survey, conclusions or attributions on inputs and policies that might have contributed to these outcomes are difficult to draw.
The NFHS has 42 indicators related to child health and nutrition. The trends in neonatal and infant mortality rates from 2015 to 2019 suggest that India has managed to reduce child mortality. Yet the major public health indicators for child health have only improved marginally or not at all, while nutrition-related indicators have worsened in most states. These include stunting (13 out of 22 states and union territories saw an increase), wasting (12 states and union territories saw an increase), underweight (16 states and union territories saw an increase), anemia (16 states and union territories saw an increase), and obesity (all states and union territories except Goa saw an increase).
NFHS-5 child nutrition story
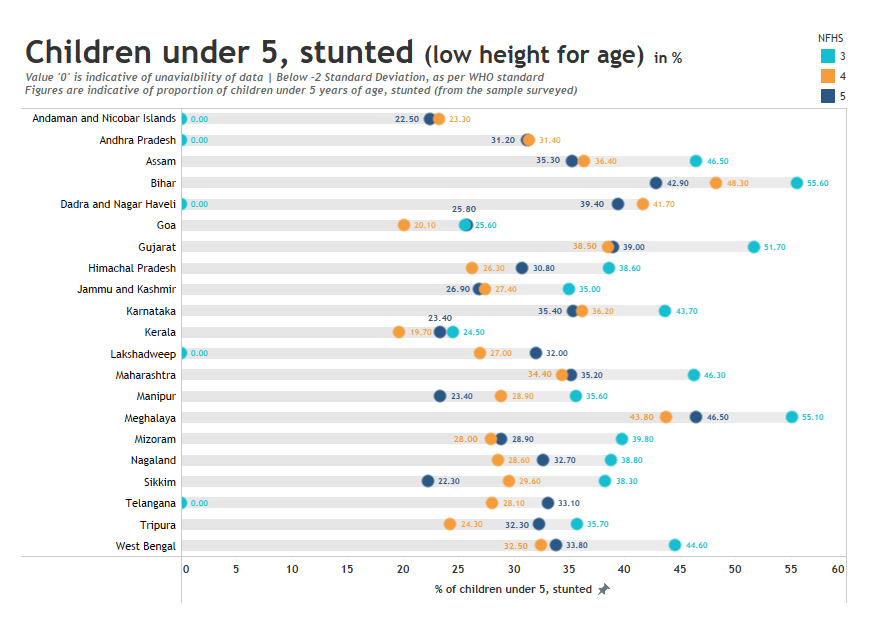
Stunting: The level of stunting, or lower-than-expected height for age, has either deteriorated or improved only marginally in most states and union territories, as compared to NFHS-4 (2015-16). Out of the states surveyed, the levels of stunting worsened in 11 states while others recorded a marginal improvement. The rates of stunting went up significantly in the states of Goa, Kerala, Telangana, and Himachal Pradesh. Tripura emerged as the worst-performing state on the indicator, with a rise from 24.3% to 32.3% in the last four years. Bihar, which had the highest levels of stunting in NFHS-4, saw a marginal decline from 48.3% to 42.9%.
The National Family Health Survey (NFHS) survey is a large-scale nationwide survey of households. The ministry has designated the International Institute of Population Sciences as the nodal agency. Fifth in the series, the factsheet released for states and union territories provides aggregated data on 131 parameters. NFHS-3 was conducted in 2005-06 and NFHS-4 in 2015-16.
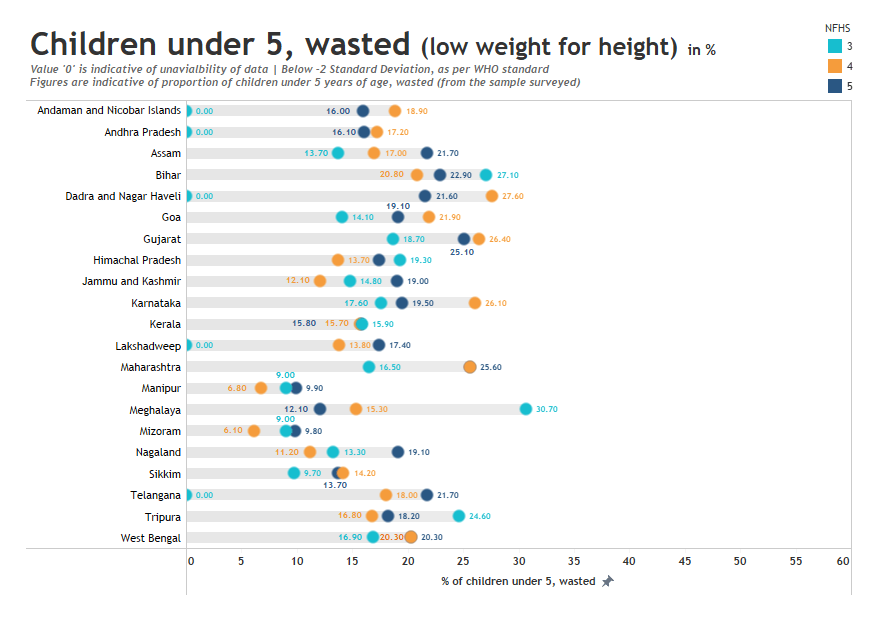
Wasting: The levels of wasting, or lower-than-expected weight for height, saw a similar trend of reversal or stagnation in most states. Of the 21 states and union territories, 10 have reversed on the parameter and the figures are closer to the levels in NFHS-3 (2005-06). Nagaland and the union territories of Jammu and Kashmir increased by six percentage basis points. With a drop from 26.1% to 19.5%, Karnataka emerged as the best-performing state. The states of Meghalaya and Goa also improved as compared to the previous survey.
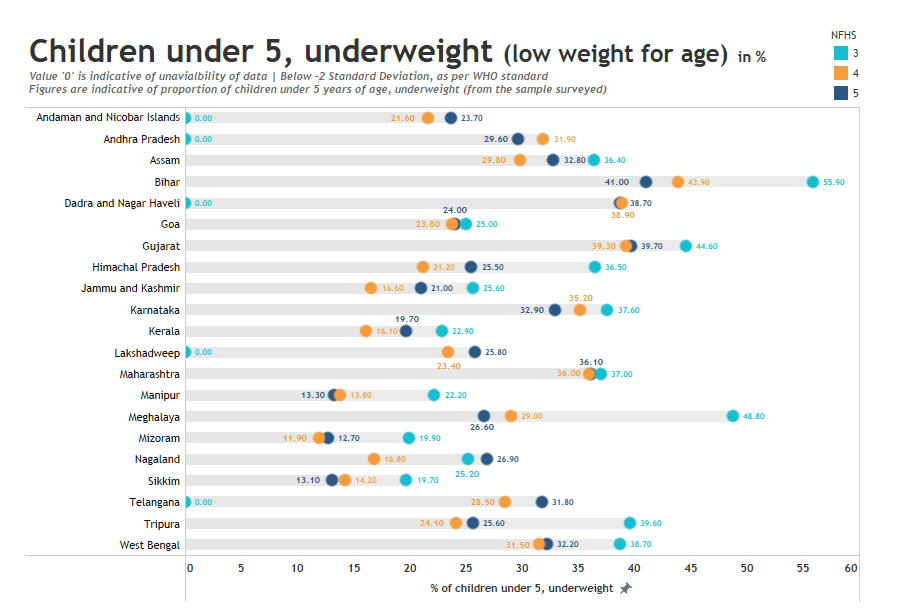
Underweight: Another indicator used to gauge the status of child nutrition is the percentage of underweight children aged five or less. This indicator also showed alarming trends similar to other nutrition parameters. The population of underweight children increased in 11 states and all five union territories. Bihar, Gujarat, and a few northeastern (NE) states saw a marginal to low decline in the levels. However, more affluent states like Kerala and Telangana saw a rise in the proportion of underweight children by almost three percentage basis points. The levels went up from 16.1% to 19.7% in Kerala and from 28.5% to 31.8% in Telangana.
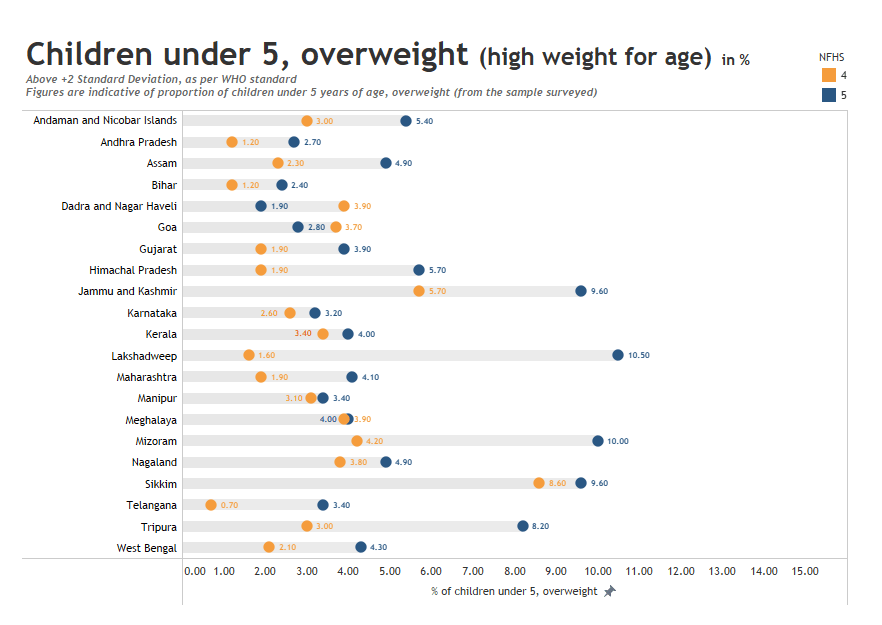
Overweight: Children aged under five are considered overweight if their weight-for-height is two standard deviations above the median of WHO’s Child Growth Standards. Although the proportion in India is within the world average as per WHO, the indicator is under distress. As compared to the previous survey, 16 out of 17 states recorded an increase in the percentage of overweight children in NFHS-5.
With a decrease from 3.7% to 2.8%, Goa was the best-performing state. All other states recorded an increase in the indicator, ranging from 0.1% to 5.8%. The percentage of overweight children more than doubled in Mizoram.
The findings point to a triple burden of malnutrition in India, in terms of stunting, wasting, and child obesity.
Anemia: The increasing prevalence of anemia among children aged 6-59 months was also worrying. In some states, the prevalence is even higher than that of NFHS-3 (2005-06). For instance, the levels rose from 35.7% to 68.4% in Assam, while Gujarat recorded a 15% increase. Other states also show a major reversal from NFHS 4 levels. The analysis highlights that as compared to NFHS-4, the parameter has worsened in 17 out of the 21 states and union territories, as shown in the graph below.
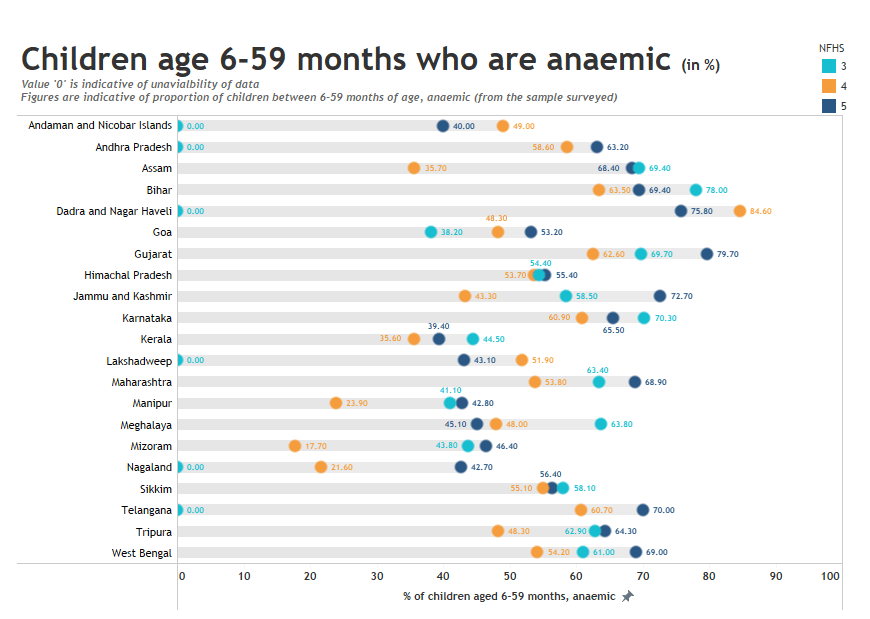
Though phase 2 data from other states will provide more clarity, these results are certainly a cause for concern and require urgent action. The second phase of NFHS-5 may present even more alarming findings since the survey was carried out after the lockdown-related restrictions were relaxed.
Underutilization of allocated resources
The government must also consider the results of the first phase of NFHS-5 in the context of India’s Mid-Day Meal (MDM) initiative. The Accountability Initiative of the Centre for Policy Research reported that only 14 states utilized 100% of the total funds allocated under MDM in 2018-19, which indicates sub-optimal performance on the ground. Another analysis by the Accountability Initiative shows that only 44% of the government-approved amount for Integrated Child Development Services (ICDS) was utilized in 2018-19. Furthermore, the number of children aged six months to six years who receive benefits under the Supplementary Nutrition Programme (SNP) was less than half the estimated number of beneficiaries in 21 states and union territories between 2017 and 2019.
The economic slowdown and stagnation in wages of the poor have translated to lower consumption, as evident from the expenditure survey of NSSO (2017-18). In this context, the results of NFHS-5 will likely reflect the reduced ability of the poor to access quality nutrition and the inadequate contribution to programs, such as ICDS and MDM, which advance better nutrition.
Need for enhanced focus on nutrition due to COVID-19
The COVID-19 pandemic has the makings of a perfect storm for the existing nutrition crisis. According to the India Child Well-being Report 2020 of World Vision India, more than 115 million children in the country no longer have three meals a day and many continue to miss mid-day meals as schools remain closed. This will have long-term adverse effects on the economic prospects of the country due to reduced schooling and cognitive impairments, and the consequent loss in productivity.
New estimates by Derek Headey and colleagues in The Lancet suggest that without timely action, the global prevalence of child wasting could rise by a shocking 14.3%. In the face of a drastic decline in income, the poor would stop consuming the more expensive nutrient-rich foods to preserve their caloric intake. This would exacerbate the undernutrition crisis. For the poorest and the most vulnerable of India, the effects could be particularly detrimental.
Dalberg’s survey of 47,000 poor households highlights the devastating economic impacts during the lockdown imposed to curb the spread of COVID-19. Primary income earners in two-thirds of surveyed households in the LMI segment lost their jobs or wages during the lockdown, and the average family lost more than 60% of their pre-crisis income. The economic distress, coupled with the halt in the mid-day meal initiative, is expected to lead to a dangerous deterioration in dietary quality.
While the ministry is yet to release granular data for all states and union territories, the consistent reversal on several parameters that gauge child nutrition is apparent from the phase 1 data. The overall trends suggest an improvement in many input indicators, such as access to sanitation, use of cleaner fuels, immunization, maternal health check-ups, exclusive breastfeeding, and adequacy of the diet. Other social determinants of health, including indicators of women’s empowerment, have also improved. However, more focused policy analysis, revised policies, and institutional overhaul are needed to identify and address the multidimensional aspects of child malnutrition.
The drop in performance across child nutrition indicators is a wake-up call for India. The country must take proactive measures and scale-up innovations to address malnutrition. Going forward, the government needs to work on certain quick fixes to address the issue of malnutrition. These could include:
- Dietary diversification at the household level, as part of the national nutrition strategy for effective supplementation of micronutrients;
- Launch and scale-up of innovations with a focus on improvement in healthcare and nutrition among children. These would include the promotion of exclusive breastfeeding, food fortification across PDS, ICDS, and MDM, enhanced care, referrals and management of severely undernourished and sick children, effective implementation of Vitamin A supplements to children up to the age of five, and regular deworming;
- Enhanced emphasis on nutrition literacy at the household level;
- Adoption of alternate delivery channels like cash transfer pilots in high-burden districts to encourage dietary diversification.
References;
[1] The National Family Health Survey (NFHS) survey is a large-scale nationwide survey of households. The ministry has designated the International Institute of Population Sciences as the nodal agency. Fifth in the series, the factsheet released for states and union territories provides aggregated data on 131 parameters. NFHS-3 was conducted in 2005-06 and NFHS-4 in 2015-16.




Leave comments