Nutrition literacy: Charting a new path forward
 by Neha Parakh, Dr. Puneet Khanduja, Mitul Thapliyal and Vijay Ravi
by Neha Parakh, Dr. Puneet Khanduja, Mitul Thapliyal and Vijay Ravi Jan 31, 2020
Jan 31, 2020 5 min
5 min
This blog examines the factors that influence people’s food choices and thus their nutritional intake. It also highlights the need for nutrition literacy among the PDS beneficiaries.
In our previous blogs 1 and 2 in this series, we discussed the sub-par nutrition statistics of India along with a lack of diversity in the dietary habit among people. We also looked at the steps the government should take to address these issues. In this blog, we highlight the importance of nutrition literacy.
MSC concluded a study in August, 2019 that assessed the nutritional gaps at the household level. The study revealed that while a minimal number of beneficiaries faced a shortage of food, the diet across all demographic groups was deficient in major macro and micronutrients. This deficiency can be attributed to the lack of diversity in the diet of the beneficiaries. People, in general, only possess a traditional knowledge of nutrition. Hence, nutrition literacy and constant “nudging” is required to improve the overall nutritional outcomes.
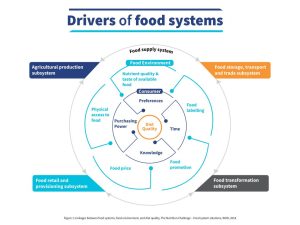
Multiple variables, termed “lifestyle factors” influence the eating habits and food choices of people, which in turn affect nutritional intake. We found that people prefer readily-available food items and the availability is influenced by agricultural economics, logistics, and market dynamics. The second level of factors that influence choice includes price, packaging, taste, and access while the third level includes knowledge, affordability, and personal preference. The diagram below illustrates the factors involved in the food supply system that affect the nutritional outcomes for individuals.
Unhealthy diets often result in malnutrition and are the cause of more adult deaths and disabilities globally than the use of alcohol and tobacco. The current food systems in India do not provide diverse and healthy diets1 for the beneficiaries and this contributes to malnutrition. All segments of society, particularly the low and middle income (LMI) segment, grapple with malnutrition. The triple burden of malnutrition—stunting and wasting, anemia, and obesity are common in women, men, and children but are especially prevalent among women and children.
Policymakers around the world have started to take the problem seriously. The annual expenditure of 25 countries for nutrition-sensitive and nutrition-specific allocations has increased to USD 16.2 billion 2,3 , in 2018. Evidence from across the globe suggests that an improved income and the availability of quality food does not necessarily translate into a marked increase in the nutrition indicators of the LMI population 4. People tend to focus on quantity rather than the quality of consumption as they are unaware of good nutrition practices.
Initiatives by the government and gaps in implementation
The Government of India (GoI) administers various programs to address issues in hunger and nutrition, such as PDS, Integrated Child Development Services (ICDS), Mid-day Meal (MDM), Poshan Abhiyan, Anemia Mukt Bharat, and the Rashtriya Poshan Maah (National Nutrition Month). While these initiatives have admirable objectives, the focus on nutrition and monitoring needs to be improved. Food fortification is a possible method to improve nutrition but it is not a desirable solution in the long term as it does not substitute for a wholesome diet. 5,6 The government also runs programs like the Village Health Sanitation Nutrition Committee (VHSNC) that use a “softer” approach to undernutrition. However, several reports highlight the gaps in implementation with regard to training, support, and monitoring in these programs 7,8,9,10.
The primary research conducted by MSC revealed that a lack of variety in the diet, along with poor choices in food, leads to high consumption of carbohydrates. People are often misled by advertisements that flaunt a “healthy” or “nutritious” label. Nutrition literacy 11 is an important lever to ensure that the beneficiaries reap the full benefits of various government initiatives and this can ultimately help drive the desired change.
Charting a new path forward
In addition to changes, such as food fortification and the introduction of variety in the PDS food basket, the government should also focus on nutrition literacy. The proper dissemination of information will help ensure the uptake of a variety of grains through PDS. The principles of behavioral science should be used to introduce nutrition literacy and ensure desirable solutions. We have provided some recommendations below to incorporate nutrition literacy through the existing channels:
i. Use the concept of orality 12 to display pictorial information on the ration cards about the healthier food items available in the PDS basket along with their associated benefits.
ii. Use the mobile numbers linked to the beneficiaries to create a messaging (SMS) platform to promote content related to health and share interactive voice response.
iii. Provide better training on nutrition to government workers at the village level, such as Anganwadi workers and ASHAs. These frontline workers should explain the health benefits of different food items to the adults and the children and use appropriate channels to disseminate tailored content to their audience, such as songs and stories for children. Anganwadi workers should use tablets to deliver messages using behavioral nudges. 13,14
iv. Strengthen initiatives like the School Health Program and monitor their implementation closely. Expand the scope of the program to include private schools to increase the outreach. Use behavioral nudges and innovative learning techniques in the curriculum, such as interactive games and competitions.
v.The government should increase its workforce to ensure the proper implementation of initiatives, such as the Poshan Abhiyan, Village Health Nutrition and Sanitation Committee, and the Scheme for Adolescent Girls. Rather than targeting just the vulnerable groups, the focus should expand to include men of the household and the elderly who may have a larger say in the food decisions in a family.
Over the past decade, nutrition has received much-needed recognition. Knowledge sharing on the topic has been significant, particularly among the middle and upper classes. However, this awareness and knowledge have not percolated to the LMI segment where undernutrition remains a challenge. A possible solution is to use Social Behavior Change Communication (SBCC) to influence the behavior of the people since it has proven more effective than traditional communication. The concept of nutrition should be introduced to the masses at an early age to create awareness and encourage acceptance. This would lead to good practices in their diets, so the evils of undernutrition can finally be stamped out.
References:
- The Nutrition Challenge – Food system solutions, WHO, 2018.
- Global nutrition report.
- This does not include food security programs, such as the public distribution system of India that alone has an annual budget of around USD 25 billion.
- Narrowing the nutrition gap.
- Guidelines on food fortification with micronutrients, WHO, FAO, 2006.
- Behavior change for better health: nutrition, hygiene and sustainability, BMC Public Health, 2013.
- Are village health sanitation and nutrition committees fulfilling their roles for decentralized. health planning and action? A mixed methods study from rural eastern India, BMC Public Health, 2016.
- Assessment of Village Health Sanitation and Nutrition Committees of Chandigarh, Indian Journal of Public Health, 2017.
- Assessment of village health sanitation and nutrition committee under NRHM in Nainital district of Uttarakhand, Indian Journal of Community Health, 2013.
- Poshan Abhiyan, Government policies and interventions for development in various sectors and issues arising out of their design and implementation, Insights Mindmaps, 2018.
- Nutrition literacy refers to the set of abilities needed to understand the importance of good nutrition to maintain health.
- Orality is the concept of simplifying communication to make it easy to understand for someone who does not read or write. It is an effective tool that focuses on the receiver and makes messages relatable and retentive.
- Study identifies the best healthy eating nudges, Eurekalert, 2019
- The Rise of “Nudge” and the Use of Behavioral Economics in Food and Health Policy, Mercatus, 2015
Written by

Neha Parakh
Analyst
Dr. Puneet Khanduja
Associate Partner
Mitul Thapliyal
Managing Partner
Leave comments